New
Special Offers For: Pediatric Children's Dentistry + Braces for All Ages. Limited Time Offer
Open ’til 7pm + Saturday
Call Us
832-804-7427
832-804-7427
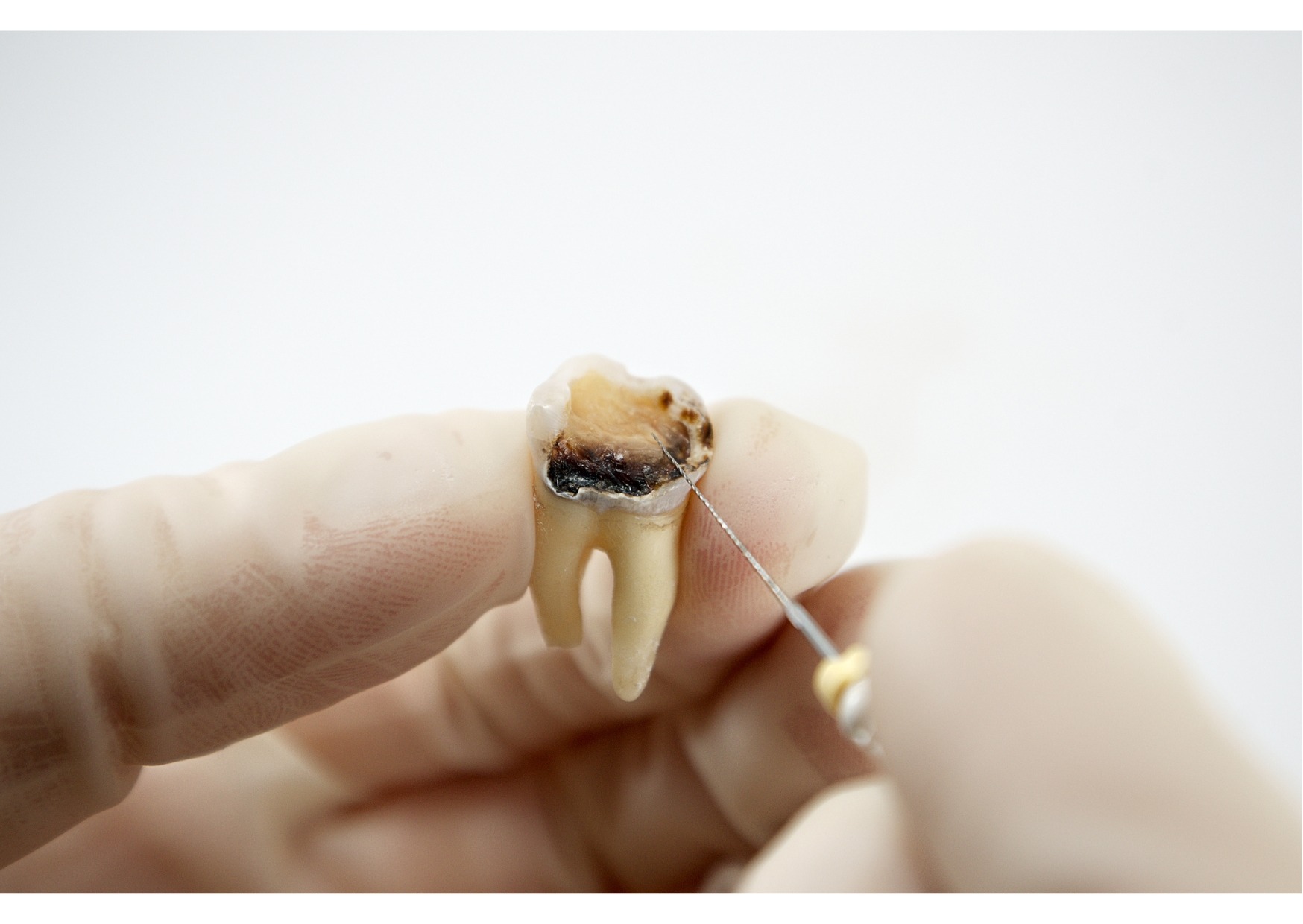
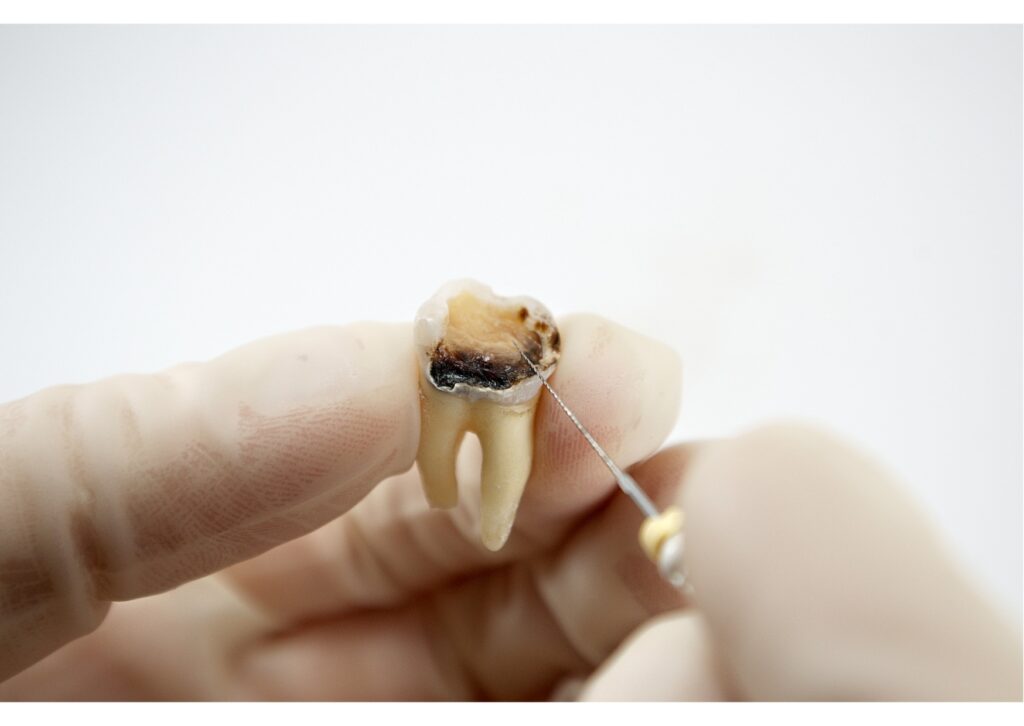
A tooth can lose its blood supply and nerve function and then remain in the mouth for weeks, months, or sometimes much longer. That may sound surprising, and it helps explain why some people delay care. The problem is that a dead tooth can seem quiet while damage continues below the surface.
Dentists usually call this a non-vital tooth. In plain language, that means the pulp inside the tooth, the soft tissue that contains nerves and blood vessels is no longer alive. Once that happens, the tooth cannot heal itself from the inside. It may stay stable for a period of time, but it also becomes more vulnerable to infection, discoloration, and cracking.
So what is the honest answer? A dead tooth can sometimes stay in the mouth for quite a while, but there is no reliable safe timeline. Some teeth become painful quickly. Others stay silent until an X-ray shows bone loss around the root, or until the tooth breaks while chewing something ordinary like crusty bread, nuts, or ice.
That uncertainty is why dentists focus less on the calendar and more on the condition of the tooth, the surrounding bone, and whether infection is present.
At Lovett Dental in Houston, TX, patients with signs of a non-vital tooth can receive a thorough evaluation and guidance on whether root canal treatment may help preserve the tooth. Our team provides patient-centered care and same-day appointment options for many individuals seeking answers about changes in tooth color, pain, or possible infection.
A healthy tooth is not just enamel and dentin. At the center is pulp, which contains blood vessels, connective tissue, and nerves. If that tissue dies, the tooth no longer has a normal internal blood supply. This can happen after a blow to the mouth, untreated decay, a deep crack, or irritation that builds over time.
In practice, dentists often see two broad patterns. One is a tooth that dies after obvious trauma, such as a sports injury, a fall, or a hit to the mouth. The other is a slower process, where a cavity, leaking filling, or crack allows bacteria to reach the pulp over time. In both situations, the tooth may become non-vital, but the next steps are not always the same.
A dead tooth is not always infected at the exact moment the pulp dies. However, dead tissue inside a tooth can create conditions where bacteria can grow. That is why a tooth may seem manageable for a while and then later develop swelling, tenderness, or a bad taste.
One of the most misleading parts of this problem is that pain may fade. People often assume that less pain means the tooth is improving. In reality, pain can lessen because the nerve tissue has died, not because the tooth has recovered.
That is why a dead tooth may remain in the mouth without dramatic symptoms for a period of time. The body may slowly wall off the area near the root tip. In some cases, changes are visible only on dental X-rays. A dentist may find a dark area around the root, which can suggest inflammation or infection in the bone.
There is also a mechanical side to the story. A non-vital tooth can become more brittle over time, especially if a large cavity, old filling, or crack is already present. So even if infection is not causing obvious symptoms yet, the tooth may still be weakening structurally.
If the question is whether a dead tooth can stay in the mouth for years, the answer is yes, sometimes. Dentists do occasionally see non-vital teeth that have been present for a long time. But that should not be taken as reassurance that waiting is safe.
The more useful question is whether the tooth is stable, restorable, and free of active infection. A tooth that has died but is treated with root canal treatment and properly restored may stay functional for many years. A tooth that is left untreated may also remain in place for a while, but the risk profile is very different.
This is where many people get tripped up. They look for a number, such as six months or two years, when dentistry works more like risk management. The longer a dead tooth remains untreated, the more opportunities there are for infection, bone loss, or fracture. None of those complications become easier to deal with by waiting.
A dead tooth often changes color. It may turn gray, yellow-brown, or darker than neighboring teeth. That color shift happens because internal tissue breakdown products can alter the way light passes through the tooth.
Other warning signs may include pain when biting, tenderness in the gum above the tooth, swelling, a pimple-like bump on the gum, a foul taste, or intermittent drainage. A bump on the gum can act like a small drainage tract from infection near the root. It may come and go, which can make the problem seem less serious than it is.
Sometimes the first sign is not pain at all. It may be a tooth that suddenly chips, a crown that loosens, or a routine exam where the dentist finds a radiolucency, meaning a dark area on X-ray that suggests bone changes around the root tip. That is one reason regular exams still matter even when symptoms are mild. For a fuller list of warning symptoms, see our root canal signs.
Some situations need prompt care rather than watchful waiting. Emergency dental care is appropriate for facial swelling or signs of spreading infection, and in some cases emergency medical care may be required. This is especially true if swelling is increasing or the area feels firm or hot, or if you have a fever. Mayo Clinic outlines these emergency signs clearly for patients.
Other red flags include trouble swallowing, trouble breathing, inability to open the mouth normally, significant swelling under the jaw, or severe pain that is escalating quickly. These symptoms can suggest that infection is moving beyond the tooth itself.
If you have an abscess and need immediate steps at home while arranging care, review dental abscess care. If you're unsure whether to seek urgent treatment, consult our dental emergency guide.
Even without dramatic swelling, persistent pain, repeated gum drainage, or a broken dead tooth should be assessed soon. A dead tooth is not automatically an emergency, but it can become one if infection spreads or the tooth fractures below the gumline.
The main treatment question is whether the tooth is restorable. If enough healthy structure remains and the root is sound, a dentist or endodontist may recommend root canal treatment. This removes the dead or infected tissue from inside the tooth, disinfects the root canal system, and seals it. After that, the tooth often needs a filling or dental crowns to protect it.
If the tooth is too damaged by decay, fracture, or severe bone loss, tooth extraction may be the safer option. That is not a failure of treatment. Sometimes removing a tooth is the most predictable way to stop infection and protect surrounding tissues. If extraction is needed, you can learn more about the tooth extraction process.
The decision is usually based on an exam, X-rays, symptoms, bite forces, crack pattern, and long-term prognosis. A front tooth darkened by old trauma may be approached differently from a heavily restored molar with a deep crack. That kind of nuance matters more than any general rule online.
This is probably the most common assumption, and it is understandable. If a tooth is not hurting, it is easy to put it at the bottom of the list. But in dentistry, silence can be deceptive.
A dead tooth may still have bacteria inside the root canal space. The body may contain that problem for a while, but not always permanently. Over time, infection can flare up, and structural weakness can become more important than symptoms.
That does not mean every non-vital tooth needs the same treatment on the same day. It does mean that a proper dental evaluation is wiser than waiting for pain to make the decision for you. Pain is only one signal, and not always the earliest or most reliable one.
Dentists do not usually diagnose a dead tooth by color alone. They combine several pieces of information. These may include a history of trauma, deep decay, temperature sensitivity, percussion tenderness, mobility, gum findings, and imaging.
A vitality test checks whether the pulp responds to cold or electrical stimulation. A lack of response may suggest the pulp is non-vital, though the result has to be interpreted in context. Research on pulp test accuracy helps explain why dentists do not rely on one test alone.
X-rays can show decay, prior dental work, cracks in some cases, and changes around the root tip.
Sometimes the story is straightforward. A tooth was hit years ago, gradually darkened, and no longer responds to vitality testing. In other cases, the diagnosis is more layered, especially when there is a crack, prior root canal treatment, or symptoms that come and go.
When a dead tooth is treated before a major fracture or extensive infection develops, the outlook is often better. Root canal treatment can remove the diseased tissue source, reduce infection risk, and allow the tooth to keep functioning.
There is also a practical benefit to acting earlier. Restoring a tooth before it breaks badly is usually simpler than trying to manage a tooth that has split or lost too much structure. In real life, that can affect cost, the number of visits, and whether replacement options become necessary. For questions about root canal longevity, read about how long treated teeth last.
For many patients, the key point is not fear but timing. A prompt exam creates options. Delay tends to narrow them.
If you think you may have a dead or non-vital tooth, do not wait for severe pain or swelling to make the decision for you. Schedule an evaluation with Lovett Dental in Houston, TX, to determine whether root canal treatment or another solution may help protect your oral health. Call +1 832-804-7427 today to book an appointment and get timely, patient-centered care.
Not safely in the sense of being ignored forever. Some dead teeth remain in place for a long time, but untreated non-vital teeth can develop infection, bone loss, discoloration, or fracture. A dentist should evaluate the tooth even if it is not painful.
No. A tooth may be non-vital without obvious active infection at that moment. Still, dead tissue inside the tooth can increase the risk of bacterial growth and later infection.
No. In fact, some dead teeth stop hurting because the nerve tissue is no longer functioning. Lack of pain does not rule out a serious problem.
Often, yes, if the tooth is structurally restorable and the root is healthy enough. Root canal treatment is a common way to preserve a non-vital tooth.
Seek urgent care if there is swelling, fever, worsening pain, drainage, a bad taste with gum swelling, trouble swallowing, trouble breathing, or difficulty opening the mouth. Those signs can suggest a more serious infection.
Lovett, Splendid & Haven Dentistry
Dental Offices in TX